Surgeon struggles to save boy’s life in L.A.’s shooting season
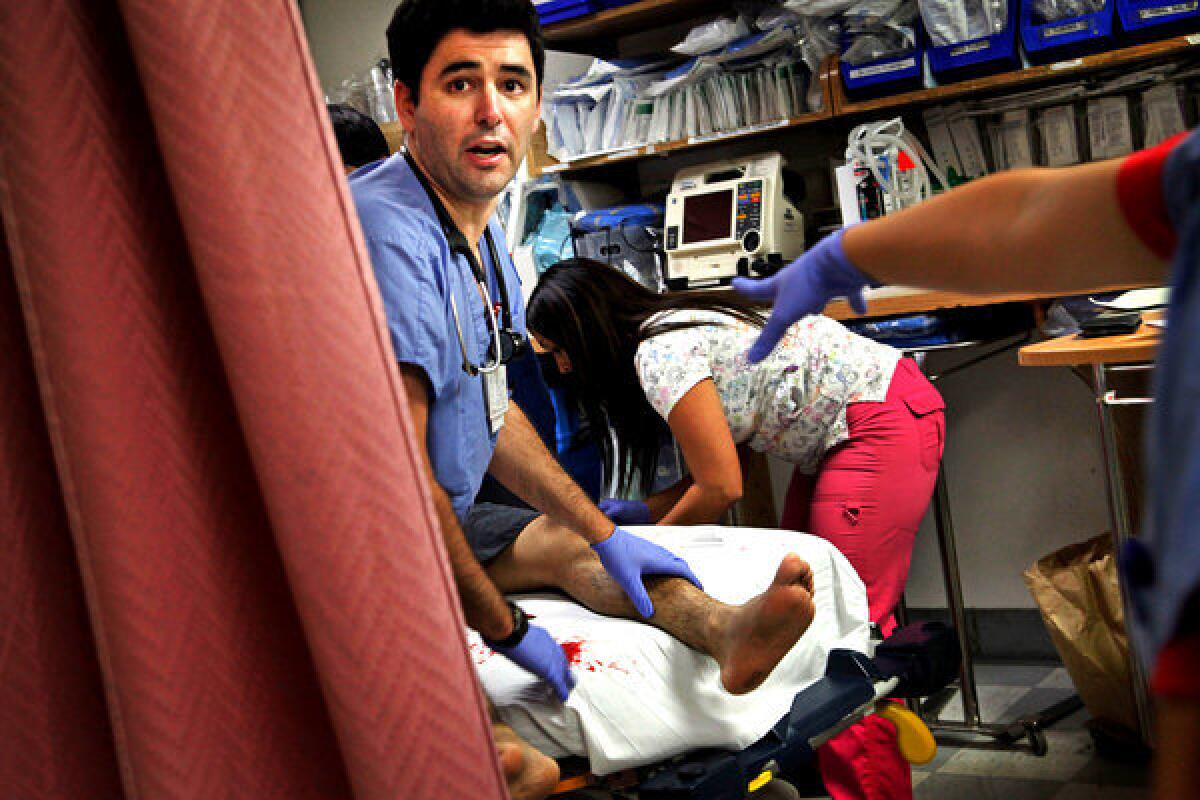
A trauma surgeon and the staff at Harbor-UCLA Medical Center race against time, trying to save a youth with a bullet in his torso.
From the entry wound — the size of a nickel — Dr. Brant Putnam guesses that the bullet is a .45, but it's what he can't see that worries him most.
The boy, a teenager most likely, lies naked on Bed 2 in a trauma bay at Harbor-UCLA Medical Center. His brown skin, slick with sweat, is ashen.
"What's your name?" a resident asks as half a dozen doctors and nurses circle him.
The boy can't answer.
"Ohhh," he moans.
"How old are you, sir?"
"Awww."
The boy's hipbones delicately protrude from his narrow waist. He has a woman's name tattooed down his right arm from elbow to wrist and the bullet hole is to the right of his navel.
Putnam, chief of trauma, stands back and watches and listens. He is puzzled that the wound is hardly bleeding.
"Sit up for me."
"Ohhh."
There is no sign of an exit wound.
"Hey. Wake up."
A resident slaps the boy. They need him conscious.
Putnam knows the surge of adrenaline that brought the boy this far is nearly spent. If his blood pressure crashes, his heart will stop. Putnam wonders if it is too late.
"Let's go to the OR," he says, loud enough to get everyone's attention.

The season of shootings has begun on time. Last year, from July through September, this Torrance hospital treated 107 gunshot victims, the highest number in the county.
This year, four GSWs — medical shorthand for gunshot wounds — arrived on the first day of summer. One was a suicide and three were assaults. Three died and one would probably be discharged in a few days.
Now, on June 23, two more have come in, both teenagers, both assaults. They walked through the front door at 2:25 a.m., no EMTs, no police. The hospital staff calls it the homeboy ambulance service: patients brought in with injuries often from gang shootings.
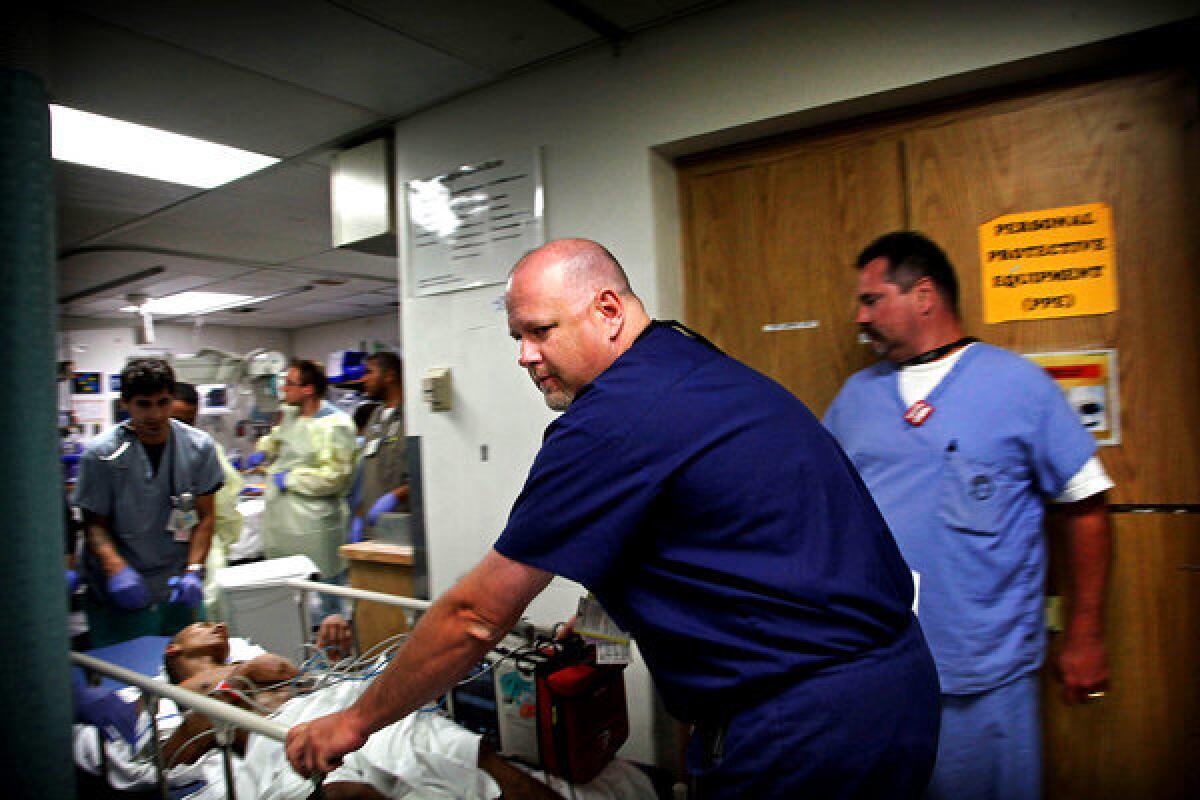
Putnam helps wheel the wounded youth to the operating room. More photos
Putnam can see that one of the boys will be OK. He has a clean wound through the shoulder.
The boy with the nickel-sized bullet hole is far worse, and they know nothing about him. No name, no age, no family. For now, they call him Zinc, one of the pseudonyms the hospital uses for its John Does.
Emergency departments in hospitals throughout America have physicians like Putnam, doctors who specialize in saving the lives of shooting victims.
Other traumas, like concussions and automobile accidents, can be subtle and require imaging to see what's hidden. Gun injuries don't hide their tracks, but they are just as much a mystery, a puzzle put together by the surgeon as seconds race by.
No matter the clarity of the injury, the damage can extend like concentric rings beyond the trajectory of the bullet. There is the blast effect, the sometimes fatal bruising that can occur to organs in the vicinity of a wound. There is the so-called triad of death, the interplay between body temperature, blood acidity and coagulation.
There is ancillary debris — shards of glass, pieces of clothing, even upholstery if the bullet has passed through furniture — and there are always infections from bacteria carried into the wound.
Putnam, 44, estimates that he has treated about 5,000 GSWs and consulted on nearly 2,000 more over the last 20 years, 10 of them at Harbor-UCLA. The victims he remembers the most are the children and women, the bystanders hit by stray fire, the wounded who spoke to him in the ER but died in the operating room.
Whenever he loses a patient, he hears his mother asking him what he could have done differently. And whenever he saves a life, he knows that success is often just a matter of luck.
Medicine and technology have come far in recent years in balancing the odds, but when it comes to gun violence, the numbers are overwhelming.
"Why guns?" Putnam asks. "Why so many guns? It once was fistfights. It once was stabbings. Now it's a whole new world out there, and with guns, it's just too much."

The emergency room team washes the boy with an antiseptic. He has been intubated and anesthetized. Blood transfusions have begun.
"Sticky blues," Putnam calls out. No time to wait for the antiseptic to dry. Nurses drape blue cloths around the boy until he disappears, with only a torso remaining.
Putnam, dressed in surgical scrubs, gloves, cap and headlamp, makes the initial incision from sternum to pubic bone, bowing around the navel.
Chief resident Carrie Luu follows the scalpel with a "Bovie," a pen-shaped tool that cauterizes the open blood vessels with electrical current. The air smells of singed flesh; tendrils of smoke rise into the lights.
Putnam sets a clock running in his mind. Two hours is optimum. Three is the limit. Anything longer compounds the trauma with a phenomena known as physiologic exhaustion, when the body has worn itself out trying to compensate for the injury.
Putnam and Luu begin by separating the small intestine and colon from their ligaments. They notice a few holes in the bowel, but those repairs can come later.
Lifting the intestine out of the torso, they find a pool of blood the size of a football flooding the back of the abdomen. This explains why the entry wound was dry. The boy is losing more blood than they can give him. Putnam wonders again if they are too late.
He orders more transfusions. A resident begins suctioning the abdomen.
"Minus 8," a nurse calls out. It's a measure of the blood's acidity, a reminder of the triad of death. A normal reading — zero — means blood clots can form naturally.
As patients lose blood, lactic acid accumulates in the cells, and the enzyme that helps coagulation doesn't function. The more acid, the more bleeding, and patients' temperatures drop until there's no stopping the loss.
Trauma teams try to interrupt this cycle. Transfusions and warming blankets help. The OR's thermostat is set as high as it will go: 85 degrees. The boy lies on a pad that's heated to 100 degrees, but still his temperature has fallen to 93.
Unable to see beyond the blood collecting in the abdomen, Putnam reaches in, and his fingers find the inferior vena cava — a vein nearly an inch in diameter — that channels blood from the lower half of the body back into the heart.
He pushes down on it, and the bleeding slows. When he eases up, he can hear a whoosh. The vena cava has been punctured.

Fired from a handgun, a .45-caliber bullet averages 900 feet per second, and unless it hits a bone, it usually follows a straight line.
This bullet's journey passed through the skin and the colon, the intestine and then the vena cava. It stopped just behind the pancreas, with its point boring nearly two inches into the spine at an angle, just missing the spinal cord.
Putnam probes the vertebra. He feels sharp fragments of bone and a hole in the L-3 vertebra no larger than his little finger. If the bullet posed a risk for pain or infection, he would remove it, but experience tells him it is safe to leave behind.
With the blood drained, he can see the damage to the vena cava: two holes in the vein, most of the tissue shredded. There will be no repairing it. Each end will have to be tied off permanently, and the other veins will have to adjust by carrying blood back to the heart.
But ligating the vena cava is tricky. Unlike arteries with their thick muscular walls, veins are as fragile as tissue paper.
Putnam puts a clamp with long pincers on the vein, which swells like a garden hose. Even in the best of circumstances, fewer than half of patients with similar injuries survive.
The boy jerks, a sudden reflex.
"Can you paralyze him so he'll stop bucking?" Putnam asks. More paralytics are added to the cocktail of intravenous drugs.
Putnam guides Luu, the chief resident, as she starts to tie off the vein. The stitch reverses direction with each pass and looks like the threads on a baseball.
"Minus 11," a nurse calls out. They have been working for almost 90 minutes.
"Come on," Putnam says, encouraging Luu. "This is where all these things really matter."
She is having trouble. Sideways torque in the needle tears out the suture. Luu is still learning — and Harbor-UCLA is a teaching hospital — but now Putnam has to take over.
"Big pledgets," he calls out, asking for the felt-like material, nearly a inch in diameter, that will act like gaskets to support each suture against the tissue. "Hurry, please."
His hands rise and fall quickly, deftly, with the grace of a pianist. His stitches, though, aren't perfect. He learned long ago that there was no call for elegance in surgeries like this. A perfect stitch could mean a dead patient.
With a little more than 12 passes, the lower portion of the vein is closed. They are almost two hours in. Putnam is sweating and splattered with blood. The room is stifling.

Emergency departments in hospitals throughout America have physicians like Putnam, center, who specialize in saving the lives of shooting victims. More photos
"Watch your eyes," Putnam announces as he removes the clamps and tests the sutures. Given the pressure in the vein, blood could spray across the room if the sutures don't hold.
They hold.
"Still very oozy," he says. The body's normal coagulants haven't begun to stop the other sources of bleeding.
He and Luu staple the top portion of the vena cava and turn to the intestine. They draw the long, serpentine tube through their hands inch by inch, stapling and stitching any tear.
A cloth is tossed on the floor to mop the blood at Putnam's feet. By now, almost 80% of the boy's blood has been replaced.
Loosely positioning the intestine inside the abdomen, Putnam begins bandaging. He won't close the incision because he plans to open the boy again in two days to reassess the work and to see how the body is healing.
"OK, we're moving," the scrub tech announces as soon as Putnam steps back and begins to strip out of his surgical gown.

Putnam remembers all the bad news he's ever delivered. He won't have to remember this one.
At 5:25 a.m., three hours after arrival, he pronounces the boy in critical condition, expected to live.
A little before 6 a.m., Putnam goes looking for the family. He still doesn't have any information about the boy.
Sleeping families fill the waiting rooms, and in the ER, Putnam speaks with the other victim, who says he doesn't know his friend's name.
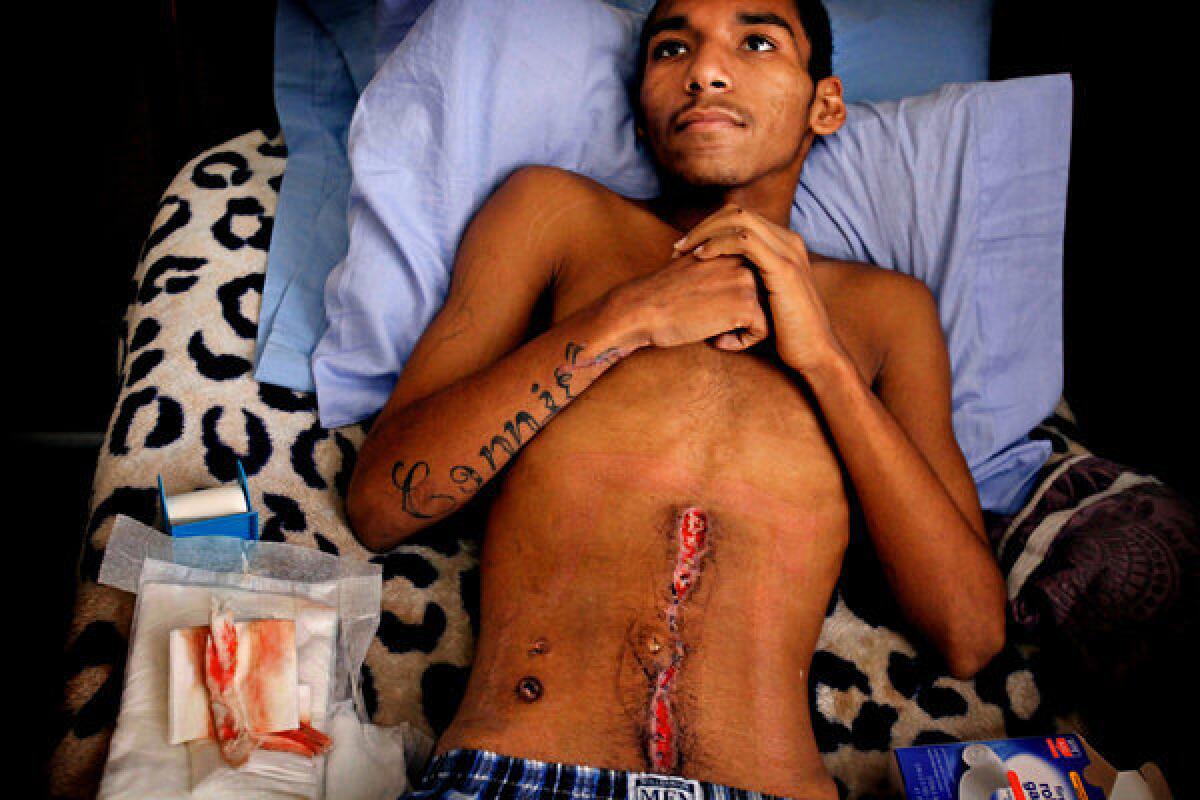
Leandrus "Lee" Benton said he was walking home from a party and thought it would be safer to cut through an alley, where he was shot. More photos
Then a call comes in. A woman is asking if the hospital has seen a young man with the name Connie tattooed on the underside of his right arm.
Within an hour, Connie Greene and her husband meet Putnam in the ICU. She is the boy's mother, and his name is Leandrus Benton. He is 16.
"He's OK," Putnam tells the parents. "He lost a lot of blood, and we almost lost him."
Connie starts to cry. In the last five years, two of her nephews have been killed in street shootings.
Leandrus — or Lee, as he's known to his family and friends — had been walking home from a party in Wilmington that night. As he would later explain, he and his friend thought it would be safer to take the alley than the street. Lee had heard the gun but didn't see the shooter. The bullet, he said, burned through his gut.
Putnam walks the couple into the ICU, and as they wash their hands, he pulls out gowns, gloves and masks for them. He then takes them to Lee, waits a minute and draws the curtain around them so they can be alone with their son.
Sign up for Essential California
The most important California stories and recommendations in your inbox every morning.
You may occasionally receive promotional content from the Los Angeles Times.








